What Are the Lateral Ankle Ligaments?
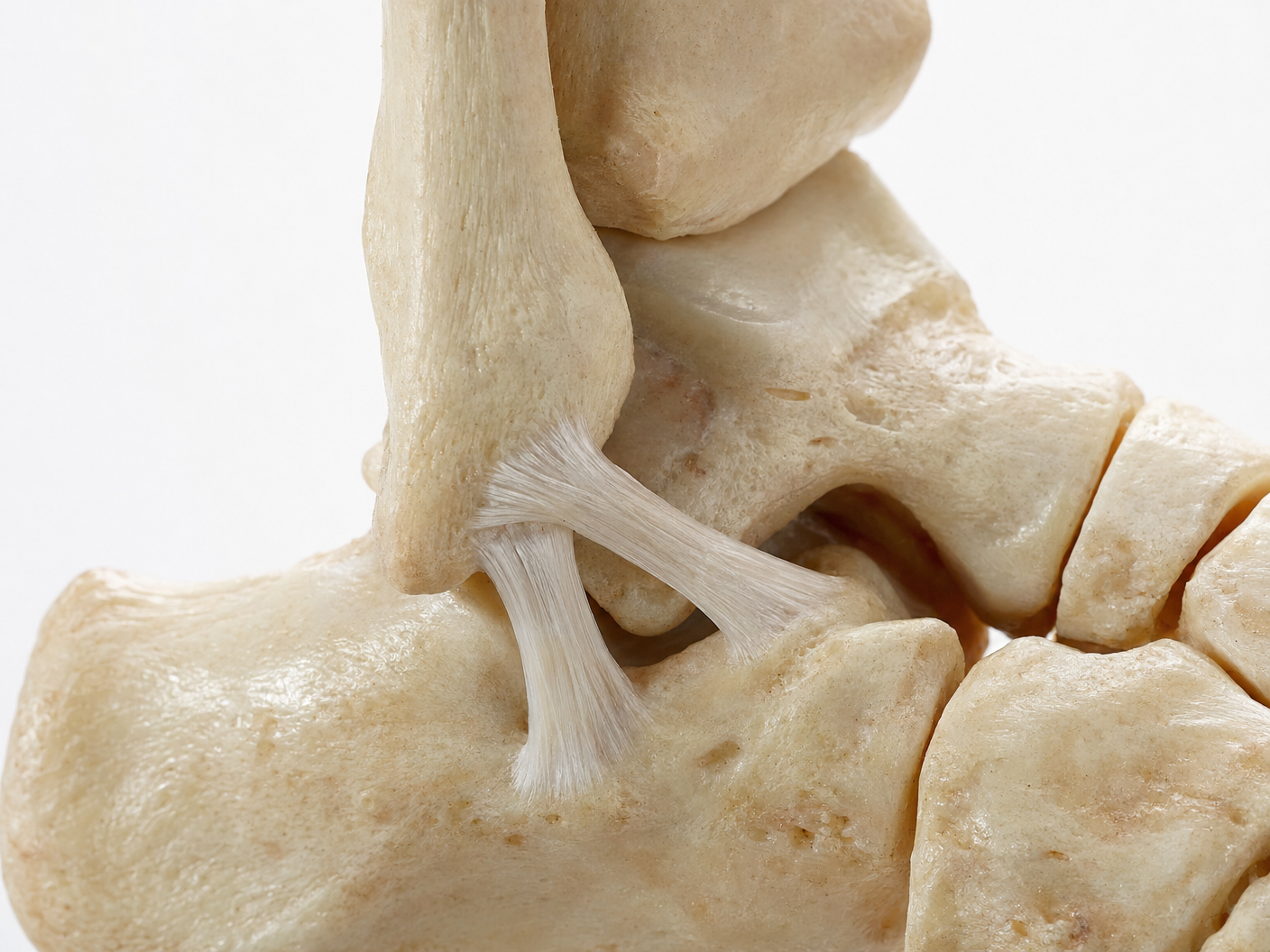
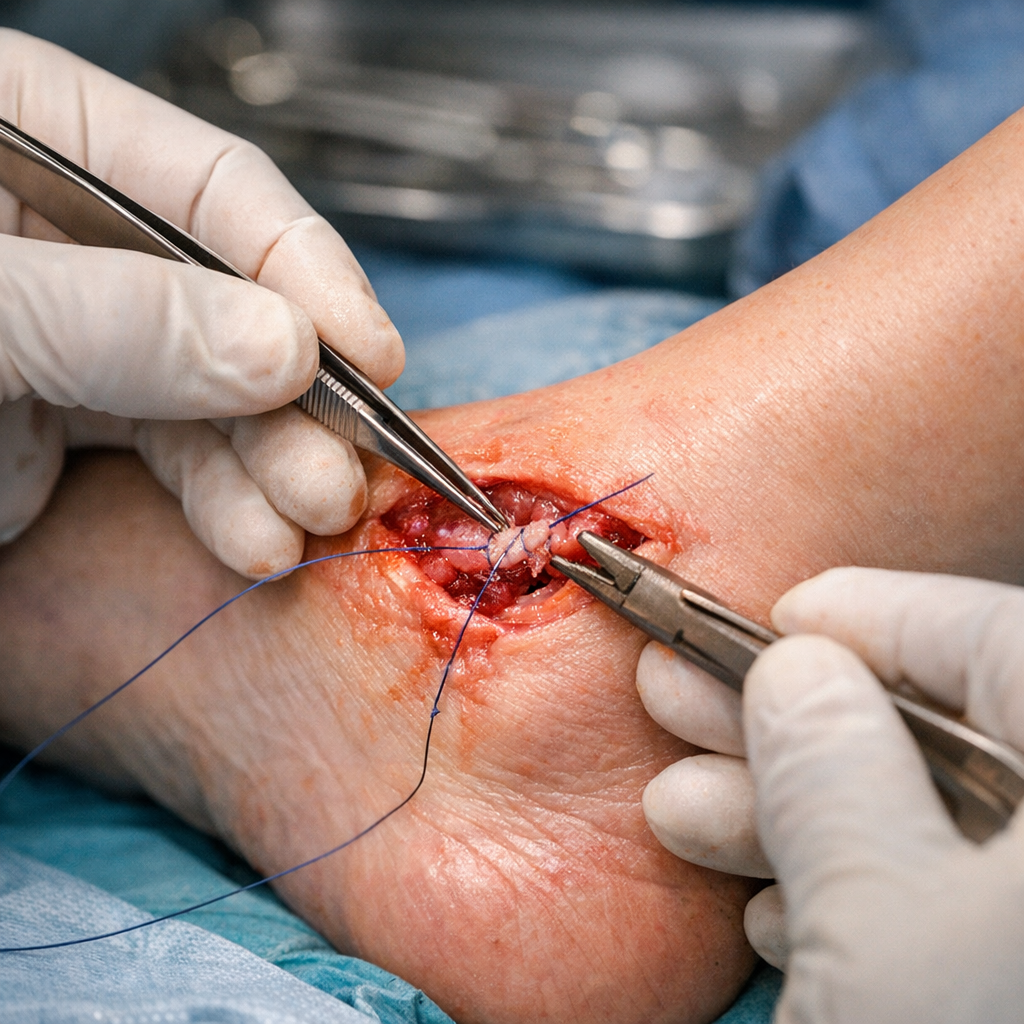
The ankle is held together by a network of strong, rope-like tissues called ligaments. On the outer (lateral) side of the ankle, three ligaments work together to prevent the ankle from rolling inward too far. The one at the front is called the anterior talofibular ligament (ATFL), which runs from the outer ankle bone (fibula) to the front of the talus — the bone that sits between the shin and the heel. The second is the calcaneofibular ligament (CFL), which connects the fibula down to the heel bone (calcaneus). The third, the posterior talofibular ligament (PTFL), sits at the back and is rarely injured except in very severe dislocations.
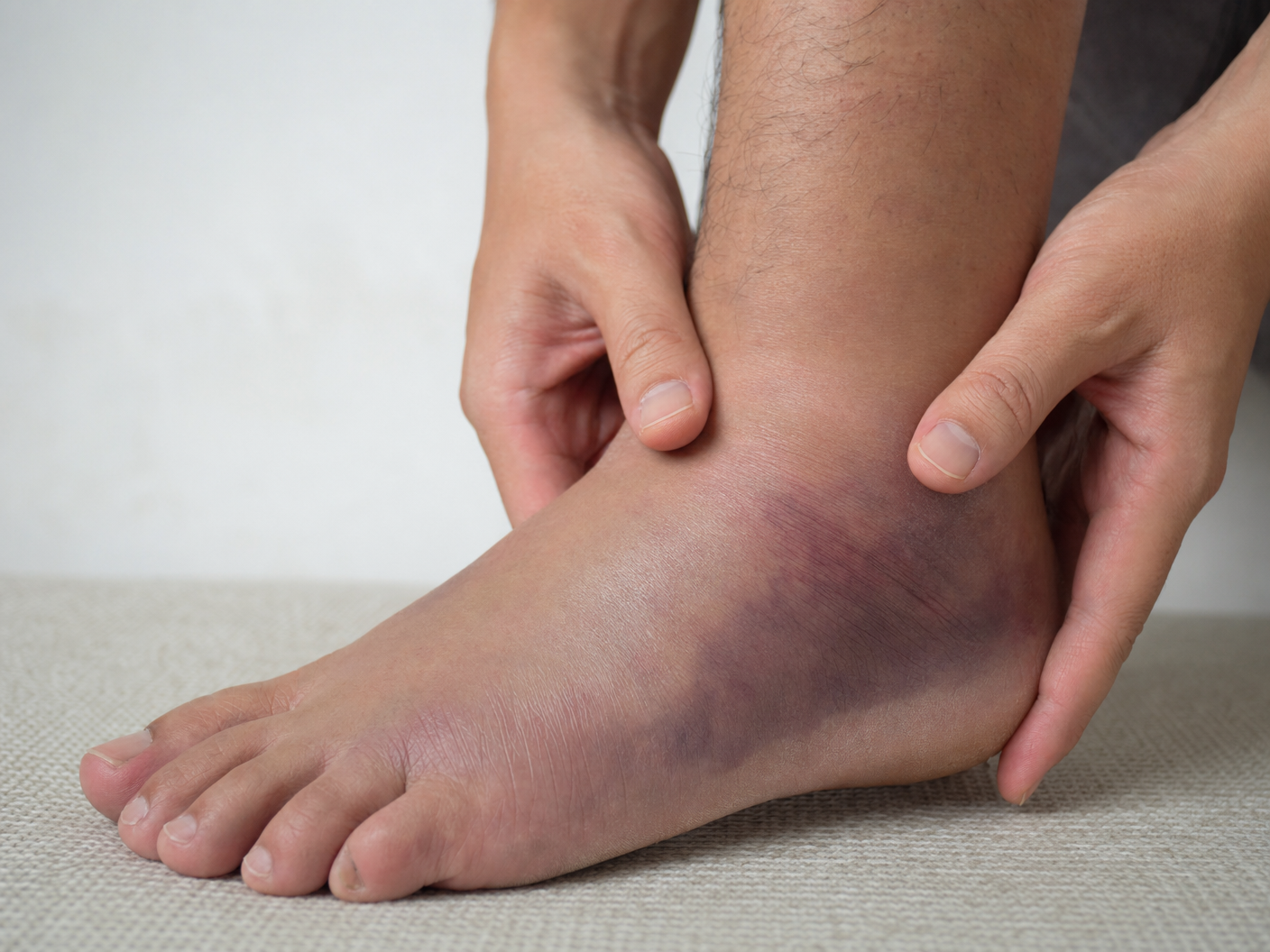
When the ankle rolls inward — the classic “twisted ankle” or ankle sprain — these ligaments can be stretched or torn. In mild sprains, the fibres are simply over-stretched; in more severe injuries, the ligament tears partially or completely. If the injury is not properly treated and rehabilitated, the ligament can heal in a lengthened position, leaving the ankle feeling unstable and prone to repeated sprains. This longer-term problem is known as chronic lateral ankle instability.
Mr Matthew Welck in London specialises in the full spectrum of ankle ligament injuries, from acute sprains through to complex reconstructive surgery for longstanding instability.